|
|
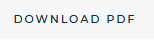
Test |
IDA |
FID |
IDA + FID |
|
Iron |
Low |
Low |
Low |
|
Ferritin |
Low |
Normal-High |
Low-Normal |
|
Transferrin |
High |
Low-Normal |
Low |
|
Transferrin saturation |
Low |
Low |
Low |
4Adapted from Weiss G, Goodnough LT. N Engl J Med 2005; 352:1011-1023
Diagnosis of Iron Deficiency
What Laboratory Tests are Needed?5
Absolute Reticulocyte Count
Both overt and functional iron deficiency are associated with decreased red cell production, manifested by reticulocytopenia. The measurement of the reticulocyte count is therefore always indicated.
For practical purposes, an absolute reticulocyte count of <75,000 in the presence of a decreased hemoglobin represents hypoproliferation (or decreased red cell production). Once increased destruction is excluded, confirmatory tests for iron deficiency should be done.
Reticulocyte Index
A convenient way to assess bone marrow response to anemia is through the reticulocyte index. A value <2 suggests a response to anemia is insufficient; a value >3 suggests an adequate response.6
Reticulocyte Hemoglobin Content (CHr, MCHr, RET-He)
Reticulocyte hemoglobin content is a direct measure of iron in the reticulocyte measured in picograms (pg). A mean CHr less than 28 pg is strongly suggestive of iron deficient erythropoiesis
Iron Status Tests
In an otherwise healthy patient (without concomitant co-morbidities), a serum iron, total iron binding capacity (TIBC), percent transferrin saturation (Fe/TIBC) and serum ferritin should suffice to diagnose iron deficiency and be strongly indicative of functional iron deficiency in the context of the patient’s clinical history. If the ferritin is elevated in the face of decreased percent transferrin saturation, a C-reactive protein as an indicator of inflammation may be useful in demonstrating that a normal or elevated ferritin is due to inflammation rather than normal iron stores.
Mean Corpuscular Volume (MCV)
The MCV can be helpful as well; however, the test lacks both sensitivity and specificity. Many patients with iron deficiency, both overt and functional, may have a normal MCV while a decreased MCV may be seen with certain hemoglobinopathies, e.g. thalassemia.
When Should Labs be Drawn?
These tests are best done fasting. There is a diurnal variation of iron levels and recent food intake can markedly affect the serum iron level, that, in turn, affects the transferrin saturation.
Symptomatic Diagnosis
If long standing iron deficiency is suspected, a simple question about ice craving (pagophagia) can be a useful screening assessment for iron deficiency. Classical physical findings include a glasslike tongue and ridged fingernails (Mees’ lines).
For more information, go to: Laboratory Studies in the Diagnosis of Iron Deficiency, Latent Iron Deficiency and Iron Deficient Erythropoiesis
Management of Absolute Iron Deficiency
Oral Iron Therapy
Consideration of oral iron remains the standard of care for the initial treatment of uncomplicated iron deficiency. A variety of enteric iron preparations are available without prescription but have been shown to vary in gastrointestinal tolerability. Listed in order of DECREASING adverse event percentage: Ferrous fumarate, ferrous sulfate, ferrous gluconate, ferrous glycine sulfate, iron protein succinylate and ferrous sulfate mucoprotease.7 Efficacy is probably equivalent.
Clinicians learn during training that oral iron is well tolerated. However, many patients complain of mild to significant adverse events and are not able to continue oral iron therapy.7
These adverse events include:7
- stomach cramping
- constipation or diarrhea
- constant metallic taste
- nausea
- sticky stool that is green and malodorous
- abdominal bloating
Recent studies suggest that alternative day oral iron supplementation may improve iron uptake, while also reducing the side effects.8
Compared to intravenous iron, oral iron is far less efficacious, takes considerably longer to work, and is ineffective in the presence of:9
- chronic diseases such as inflammatory bowel disease and other inflammatory processes
- chronic renal failure
- malabsoption disorders
- malignancies
Enteric iron replacement may be inadequate, even if tolerated, if the rate of blood loss, and therefore iron loss, exceeds the patient’s maximum rate of daily iron absorption with optimal oral iron replacement.9 This may be seen due to a reduction in iron absorption secondary to bariatric surgery or malabsorption, or significant chronic blood loss such as from gastrointestinal pathology or dysfunctional uterine bleeding.
Oral iron is contraindicated in inflammatory bowel disease where it is directly toxic to the intestinal endothelium exacerbating the inflammation.
Intravenous (IV) Iron Therapy
IV iron therapy is indicated for any patient in whom enteric iron replacement is ineffective or not tolerated. In addition, since the response to parenteral iron is much faster, clinical circumstances such as an urgent need for surgery, might dictate the medical necessity of intravenous iron. There are currently five IV iron preparations available in the US.
For more information, go to Treatment of Iron Deficiency Anemia.
References
- Coyne DW, Kapoian T, Suki W, et al. Ferric gluconate is highly efficacious in anemic hemodialysis patients with high serum ferritin and low transferrin saturation: results of the Dialysis Patients’ Response to IV iron with Elevated Ferritin (DRIVE) study. J Am Soc Nephrol. 2007; 18: 975-984.
- Wish JB. Assessing iron status: beyond serum ferritin and transferrin saturation. Clin J Am Soc Nephrol. 2006; 1(suppl 1): S4-S8.
- Macrophages and iron trafficking at the birth and death of red cells. Korolnek T, Hamza I. 2015;125(19):2893. Epub 2015 Mar 16.
- Weiss G, Goodnough LT. Anemia of Chronic Disease N Engl J Med 2005; 352:1011-1023
- Goodnough LT, Nemeth E, Ganz T, Detection, evaluation, and management of iron-restricted erythropoiesis. Blood 2010: 116(23): 4754-4761.
- Hutchinson RE, Davey FR. Hematopoiesis. In: Henry JB, ed. Clinical Diagnosis and Management by Laboratory Methods 19th edition. WB Saunders 1996.
- Cancelo-Hidalgo MJ et al, Tolerability of different oral iron supplements: a systematic review. Curr Med Res Opin .2013;29:291-303.
- Arcangelo V, Peterson A. Pharmacotherapeutics for Advanced Practice A Practical Approach. Second Edition, 2006. Philadelphia, Pa. Lippincott Williams and Wilkins. Chapter 55 Anemias (Kelly Barranger) pg 800.